Uterus Removal Surgery in Nawanshahr: 7 Signs You Shouldn’t Ignore!

REVIEWED BY Dr. Lakshita Saini (MBBS, MS Obs & Gynae) on 11th April 2026.
Have you noticed something off lately? Maybe your periods have been heavier than usual, or there’s a nagging pain in your lower abdomen that comes and goes. Perhaps your cycles have become unpredictable, and you keep telling yourself it’s just stress, or that it’ll pass. A lot of women in Nawanshahr do the same thing. They wait. They hope. And honestly, that’s understandable because the uncertainty alone can be overwhelming.
The problem is that uncertainty pulls you in two very different directions. Some women delay seeking help for far too long. Others spiral into thinking the worst, convincing themselves that surgery is already on the table. That they’ll end up losing their uterus, and that there’s no other way out.
But here’s the thing. Neither of those extremes is where most women actually land. Surgery isn’t always the answer, and in many cases, it absolutely isn’t necessary. At the same time, there are situations where a hysterectomy genuinely is the right call, and avoiding it only makes things harder down the line. The tricky part is figuring out which situation you’re actually in.
That’s what this article is really about. We’ll talk about the symptoms worth paying attention to, when surgery becomes a serious consideration, what alternatives exist, and what the whole process looks like if it does come to that.
Our goal is simple. By the time you finish reading, you should feel informed enough to have a real conversation with your doctor, without fear clouding your judgment.
What Is a Hysterectomy?

A hysterectomy is a surgery where the uterus, commonly known as the womb, is taken out. The uterus is what allows menstruation to happen and carries a baby during pregnancy, so once it’s removed, periods stop for good, and pregnancy is no longer possible.
Doctors don’t take this decision lightly, and it’s rarely the first thing they suggest. Before considering surgery, most physicians will try other routes, like medication or less invasive treatments. It only becomes a real conversation when those options haven’t helped, or when the underlying condition is too serious to keep managing conservatively.
When Is a Hysterectomy Generally Considered?
A doctor might bring up uterus removal if you’re struggling with:
- Uterine fibroids that keep causing heavy or prolonged bleeding
- Severe endometriosis that hasn’t improved with other treatments
- Uterine prolapse that makes day-to-day life difficult
- Abnormal or precancerous changes in the uterus or cervix
- Gynecological cancers
Important Factors Before Deciding on Surgery
Every situation is different, and no two patients are the same. Before recommending surgery, your doctor will think through:
- How bad your symptoms are and how long you’ve been living with them
- Your age and general health at the time
- What treatments you’ve already tried and how your body responded
- Whether having children is still something you’re considering
What Patients Should Understand
When performed for genuine medical reasons, a hysterectomy is a proven and safe surgery. Surgical methods have come a long way, which means most patients today recover faster and face fewer complications than in the past, particularly when care is in the hands of a skilled and experienced surgeon.
Surgery isn’t the automatic answer, but putting it off when it’s truly needed can make things worse over time. A thorough medical evaluation, honest conversations with your doctor, and a well-timed decision are what give you the best possible outcome.
When Do You Actually Need a Hysterectomy?
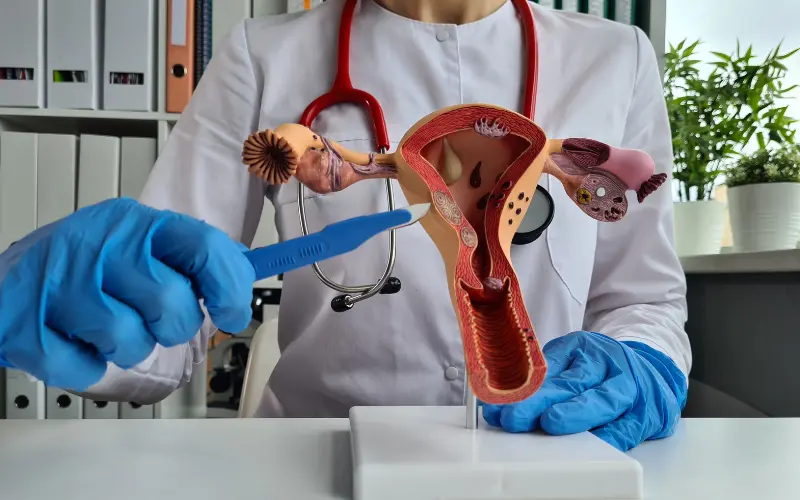
Many women hear the word “hysterectomy” and immediately feel anxious wondering if their doctor is jumping to conclusions. Honestly, that fear is understandable. But here’s what most people don’t realize: surgeons don’t take this decision lightly. It only comes up after other options have been exhausted.
Medical conditions where hysterectomy may be required
There are specific situations where this surgery genuinely makes sense:
- Uterine fibroids that won’t respond to medication and are causing heavy bleeding, pain, or a constant feeling of pressure
- Endometriosis that keeps returning or getting worse no matter what treatment is tried
- Uterine prolapse, where the uterus drops out of position and starts causing discomfort or bladder problems
- Abnormal or precancerous changes detected in the uterus or cervix
- Gynecological cancers, where surgery is often a core part of treatment
When non-surgical treatments are not enough
Surgery is rarely the first suggestion. Most doctors start with:
- Medications for bleeding or pain relief
- Hormonal therapy
- Dietary and lifestyle adjustments
- Minimally invasive procedures
But sometimes none of it holds. Surgery becomes the more serious conversation when symptoms keep escalating, when nothing has worked long-term, when daily life is genuinely suffering because of fatigue or pain, or when waiting could put someone’s health at real risk.
Situations where acting sooner matters
Putting off surgery in certain cases isn’t just uncomfortable it can backfire. Prolonged heavy bleeding can lead to severe anemia. Pain that’s manageable today can become debilitating later. And in precancerous or cancerous situations, delays can allow the disease to progress further than anyone wants.
Getting the timing right matters more than most people think.
What this means for you
Here’s the honest truth: most symptoms won’t end in surgery. But dismissing something that keeps coming back isn’t wise either. Get properly diagnosed, ask questions, and make your choice based on what your body actually needs not on fear, not on assumptions, and not on what a quick internet search tells you at midnight.
Early Symptoms You Should NOT Ignore

Many women brush off early warning signs, chalking them up to “just hormones” or getting older. But sometimes, your body is trying to tell you something more, and certain symptoms may point to underlying gynecological conditions that genuinely need attention before they get worse.
Common Warning Signs to Watch For
If any of the following sounds familiar and has been happening regularly, it’s worth having a conversation with your doctor:
- Heavy or prolonged menstrual bleeding Some women find themselves going through pads faster than normal, or their period just keeps going well past the usual days.
- Pelvic pain or pressure It might feel like a dull ache or a heaviness in your lower belly that lingers around longer than it should.
- Irregular periods Your cycle feels all over the place, or you get bleeding at times that catch you completely off guard.
- Pain during intercourse A lot of women stay quiet about this one, but it’s not something to push through or normalize without getting it checked.
- Frequent urination or difficulty emptying the bladder You might feel like you constantly need to go, or like your bladder never fully empties, which can sometimes be connected to fibroids or an enlarged uterus pressing on nearby areas.
Why Early Detection Matters
Here’s the thing: ignoring these signs doesn’t make them go away. What starts as something manageable can quietly progress into a condition that needs far more intensive treatment down the line. Catching it early opens the door to simpler, non-surgical options and generally leads to much better outcomes.
When Should You See a Doctor?
There is no perfect moment to book that appointment, but your body often gives you clear enough hints. Here are some signs that it is time to stop waiting:
- Symptoms that keep coming back or are getting worse If it is happening over and over again, or slowly building up rather than settling down, that pattern alone is worth getting checked.
- Bleeding that is affecting your daily life When your period starts deciding what you can and cannot do, whether it is going to work, stepping out, or just getting through the day, that is not something to keep adjusting around.
- Pain that interrupts your normal routine If you are skipping things or holding back because of discomfort, that is your body asking for more than just a painkiller.
- A noticeable change in your menstrual pattern Something feels different lately, the timing, the flow, the way your body feels around it. If it is new and it is staying, it deserves attention.
Getting a doctor’s opinion early does not mean bracing for the worst. More often, it simply means understanding what is going on and finding the easiest way to manage it before it becomes harder to deal with.
Can You Avoid Hysterectomy? (Lifestyle and Non-Surgical Options)

When a doctor first brings up hysterectomy, most women leave that appointment with one thing on their mind: is there another way? It is a fair question, and the answer is not always straightforward. Some women find they never need surgery at all.
Others try everything and still end up in the operating room. Where you land depends largely on what is causing the problem, how bad it has gotten, and how soon it was caught. A lot depends on what condition you are dealing with, how far along it has progressed, and when it was first identified.
Surgery tends to be a last resort, not a starting point. Most doctors will work through other options first before putting uterus removal on the table.
Non-surgical treatment options
There is no single approach that works for everyone, but depending on what you have been diagnosed with, some of these may be worth discussing with your doctor:
- Medications to control heavy bleeding or pain
- Hormonal therapy to help regulate your menstrual cycle
- An intrauterine device (IUD), which suits certain conditions well
- Minimally invasive procedures for fibroids or abnormal tissue
Catching the problem early genuinely improves how well these options tend to work.
The role of lifestyle in managing symptoms
Nobody wants to hear “eat better and exercise” when they are dealing with a real medical condition. But the reality is, how you live does show up in how your body handles treatment. A woman who is chronically stressed, barely sleeping, and eating poorly is going to have a harder time than one who is not. Small shifts in activity, food, and stress management will not fix everything, but they do matter more than most people expect.
None of this replaces actual medical care. But it can take the edge off symptoms and sometimes slow down how quickly things progress.
When hysterectomy becomes unavoidable
There are situations where non-surgical options just do not hold up. Surgery tends to become the necessary choice when symptoms keep worsening despite treatment, when nothing has brought lasting relief, when your quality of life is taking a serious hit, or when waiting any longer would put you at real risk.
What you should know going into this
Some women do successfully avoid surgery. Others cannot, and that does not mean anything went wrong. The goal is always to find what is actually going to help your specific situation, not to delay treatment just for the sake of avoiding an operation.
Types of Hysterectomy Procedures Explained

If your doctor has brought up hysterectomy as an option, one thing worth knowing early on is that this is not a single, one-size-fits-all surgery. There are actually several different types, and which one gets recommended really comes down to your specific condition, how severe your symptoms are, and your overall health going into it.
Even a basic understanding of your options can take some of the uncertainty out of what comes next.
Based on what is removed
- Total hysterectomy; The entire uterus, including the cervix, is removed. This is the most commonly performed type.
- Partial hysterectomy; Only the upper part of the uterus is removed, while the cervix is left intact. This may be considered in specific cases.
- Radical hysterectomy; This involves removal of the uterus along with surrounding tissues and is usually done in cancer-related cases.
Based on how the surgery is performed
- Laparoscopic hysterectomy; A minimally invasive procedure performed using small incisions and a camera. It generally involves less pain and faster recovery.
- Abdominal (open) hysterectomy; A traditional surgery involving a larger incision in the abdomen. It may be required in more complex cases.
- Vaginal hysterectomy; The uterus is removed through the vagina without external incisions. This is often recommended when suitable.
How the right procedure is decided
The choice of procedure depends on:
- The underlying medical condition
- Size and position of the uterus
- Patient’s medical history
- Surgeon’s assessment and expertise
An experienced gynecologist will evaluate all these factors before recommending the most appropriate and safe surgical approach.
Life After Uterus Removal: Myths vs Reality
A lot of women come into this decision carrying fear that is mostly built on misinformation. Here is what actually holds up.
Myth: Life quality reduces after hysterectomy
Reality: Many women feel significantly better afterward. Chronic pain and heavy bleeding take a real toll over time, and for most, having that resolved is a welcome change.
Myth: Hormonal balance is completely disturbed
Reality: Only if the ovaries are removed. When they are kept intact, which is common, hormones continue working as normal.
Myth: Recovery takes a very long time
Reality: Most women are back to their routine within a few weeks. Surgical techniques have improved a lot, and recovery today is much smoother than people expect.
Myth: You will feel weak permanently
Reality: Some tiredness after surgery is normal. It passes. Most women regain their strength fully with basic rest and care.
Myth: Surgery is always the only option
Reality: It is usually the last option, not the first. Medications and other treatments are tried before surgery ever comes into the picture.
What patients should understand
Most of the fear around hysterectomy comes from not having the right information. Talking openly with your gynecologist makes a bigger difference than people realize.
Why Choose Raja Hospital, Nawanshahr for Hysterectomy
Raja Hospital provides focused gynecological care with an emphasis on accurate diagnosis and patient safety. The goal is to recommend the right treatment at the right time.
Experienced Gynecologist
Dr. Lakshita specializes in managing complex gynecological conditions with a patient-first approach.
- Proper diagnosis before recommending surgery
- Personalized treatment planning
- Clear guidance at every step
Advanced Treatment Approach
Modern techniques are used to ensure safer procedures and smoother recovery.
- Minimally invasive surgery options
- Reduced pain and faster healing
- Shorter hospital stay
Patient-Focused Care
Patients are supported throughout the entire treatment journey, from consultation to recovery.
- Honest, straightforward communication at every step
- A setting where you actually feel at ease during treatment
- Someone checking in on you properly after surgery, not just sending you home
If something feels off or a doctor has mentioned surgery, getting a second opinion or the right medical advice early on can make a real difference.
Frequently Asked Questions
Is hysterectomy a safe procedure?
Yes, hysterectomy is a commonly performed and safe surgery when done under proper medical supervision. The risk of complications is low, especially with modern techniques.
What is the right age for hysterectomy?
There is no fixed age. The decision depends on the patient’s medical condition, symptoms, and overall health rather than age alone.
Will hysterectomy affect hormones?
Hormonal changes depend on whether the ovaries are removed. In many cases, ovaries are preserved, and hormonal balance remains largely unaffected.
How long does it take to recover after hysterectomy?
Recovery time varies by procedure. Most patients recover within a few weeks, while complete healing may take up to 6 to 8 weeks in some cases.
Can hysterectomy be avoided?
In some cases, yes. Early diagnosis and non-surgical treatments can help manage certain conditions. However, surgery becomes necessary when symptoms are severe or other treatments fail.
Struggling with same?
Book Your Appointment With Our Expert Doctors

Conclusion:
Honestly, the idea of uterus removal surgery scares a lot of women more than it probably should. That fear is completely understandable, but it sometimes gets in the way of making a clear-headed decision. Some gynecological conditions never even reach the point of needing surgery if they’re caught and treated early enough. Others simply won’t resolve on their own, and waiting too long can make things harder down the road.
Paying attention to what your body is telling you matters more than most people realize. Symptoms that keep showing up aren’t something to push aside or explain away. Talking to a doctor sooner rather than later gives you more options, not fewer. And once you actually have a diagnosis in hand, the whole situation tends to feel much more manageable.
Surgery, if it turns out to be necessary, isn’t the end of the conversation. It’s just one part of a larger picture that includes recovery, follow-up care, and getting back to feeling like yourself.
The right gynecologist makes a bigger difference than most people expect. Not every gynecologist approaches things the same way. Finding one who genuinely listens, walks you through your options, and keeps your specific circumstances in mind can make what feels like an overwhelming process a whole lot more manageable.
